Anatomic and Reverse Total Shoulder Replacement
Shoulder Anatomy and Arthritis
Arthritis can affect any joint in the body including the shoulder. All joints have cartilage on their surfaces including the glenohumeral joint which is the primary ball and socket joint of the shoulder. Cartilage is a smooth structure that covers the ends of the bones. In the shoulder, the top of the humerus or arm bone articulates with the glenoid cavity which is part of the scapula or shoulder blade. Both the humeral head and the glenoid are covered with cartilage. This prevents friction between the two bones. Cartilage also does not have nerve endings allowing the joint to move without pain.
When the cartilage is injured, the underlying bone becomes exposed and then the exposed bone rubs on the opposite side of the joint. The condition where the cartilage becomes injured and is no longer present is called arthritis. There are various types of arthritis including osteoarthritis and arthritis associated with rotator cuff tears (rotator cuff arthropathy). These are the two most common types of arthritis we typically will treat with joint replacement surgery. Other types of less common forms of shoulder arthritis include rheumatoid arthritis, post-traumatic arthritis and post-instability arthritis.
The types of shoulder replacement surgery include an anatomic total shoulder arthroplasty, a reverse total shoulder arthroplasty or a hemiarthroplasty. Each has its own separate indications and advantages
Shoulder Replacement Options
Anatomic Total Shoulder Arthroplasty
Anatomic total shoulder arthroplasty is performed for patients who have pain and limited function due to arthritis of the glenohumeral joint between the humerus and the glenoid with an intact group of rotator cuff muscles and no severe bone loss on the humerus or glenoid side of the joint. Mild to moderate levels of glenoid bone loss can be accommodated for with preparation techniques or augmented components (see images below). In this surgery, the humeral head is resected and replaced with a metallic replica of the humeral head and the glenoid is resurfaced with a plastic plate with pegs on the back side that are cemented into drill holes placed in the glenoid (socket) using bone cement. The head of the implant is made of an alloy of cobalt chrome and smaller amounts of other metals or titanium and the socket is made of high molecular weight polyethylene which is a type of plastic. If you have an allergy to metal where you have difficulty wearing jewelry not made of pure silver or gold, you should alert the team so we can utilize an implant made of pure titanium. Currently, we utilize stemless humeral implants if at all possible because they minimize the trauma to the humerus by not entering the humeral canal (see images below). If the quality of the proximal humeral bone is insufficient to allow a stemless implant, then we will utilize a traditional stemmed humeral component. Pain relief is extremely predictable after anatomic total shoulder arthroplasty as well as improvement in range of motion and function. We expect patients to return to almost all sport although will recommend against heavy weightlifting or contact sports or heavy manual labor.
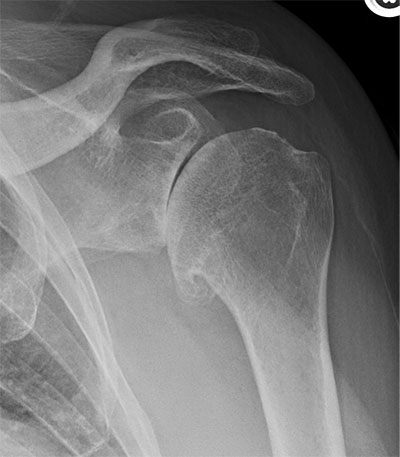
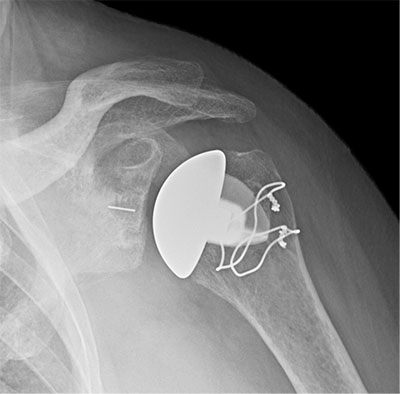
Primary glenohumeral osteoarthritis treated with a stemless anatomic total shoulder arthroplasty
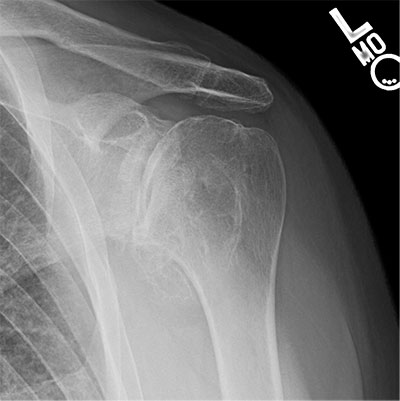
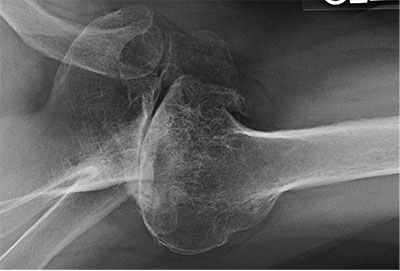
Primary glenohumeral osteoarthritis with severe posterior glenoid erosion
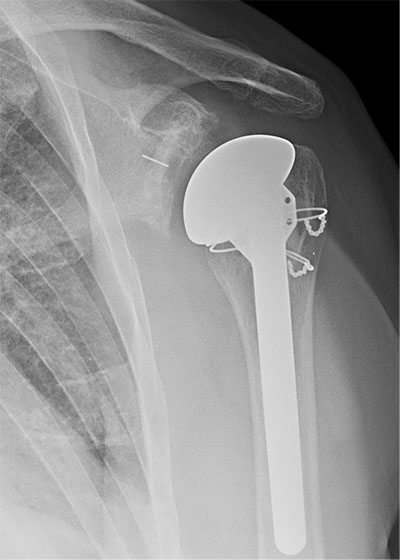
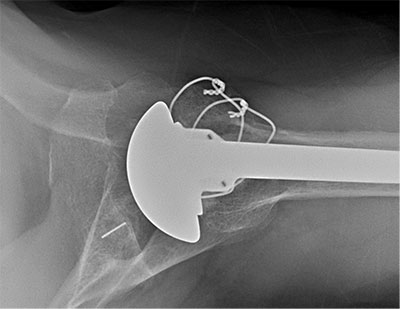
Previous patient with primary glenohumeral osteoarthritis treated with a stemmed anatomic total shoulder arthroplasty with posterior augmented glenoid component
Hemiarthroplasty
Hemiarthroplasty can be used instead of an anatomic total shoulder arthroplasty in very select cases, specifically young patients with high demands that prefer no restrictions to the shoulder postoperatively including heavy lifting, contact sports and heavy manual labor. In order to perform a hemiarthroplasty, the rotator cuff muscles need to be completely intact and there must not be any significant off-axis wear of the glenoid (socket). In the cases of hemiarthroplasty, only the humerus is replaced with either a metal humeral head or a head made of pyrocarbon. The glenoid socket is left alone. Pyrocarbon has the theoretical advantage of minimizing wear on the glenoid socket as it is not resurfaced in the setting of a hemiarthroplasty. Pyrocarbon hemiarthroplasty has been FDA approved for use in the Fall of 2020 and we will perform pyrocarbon hemiarthroplasties when they become available in appropriately indicated patients. When deciding to perform a hemiarthroplasty, patients must understand that pain control will not be as complete as when an anatomic total shoulder arthroplasty is performed although the benefit is the ability to perform unrestricted lifting including high demand manual labor in a young patient.
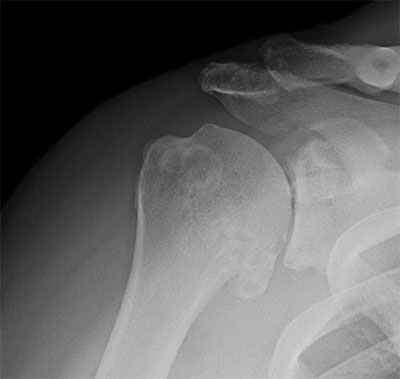
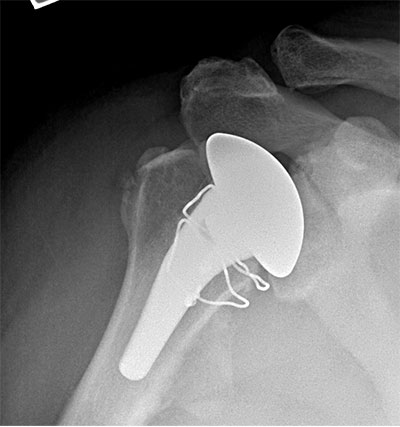
Young high demand patient with osteoarthritis without off-axis glenoid wear treated with a hemiarthroplasty
Reverse Total Shoulder Arthroplasty
Reverse total shoulder arthroplasty was originally designed for patients with rotator cuff arthropathy or arthritis of the glenohumeral joint with irreparable tearing of the rotator cuff. Prior to reverse total shoulder arthroplasty, the only option in this group of patients was a hemiarthroplasty as performing an anatomic total shoulder arthroplasty led to early glenoid component loosening and failure. Hemiarthroplasty in this group of patients often provides pain relief but active motion is often restricted with limited goals of below shoulder height activity. In the late 1980’s, the reverse total shoulder arthroplasty was developed in France and was subsequently FDA approved for usage in the United States in 2004. Currently, reverse total shoulder arthroplasty is the most commonly performed type of shoulder arthroplasty due to its flexibility in treating a variety of shoulder pathologies.
The original diagnosis treated by a reverse total shoulder arthroplasty was shoulder arthritis in the setting of an irreparable rotator cuff tear. Patients often have very limited ability to raise the arm and the mechanics of the replacement allow the patient to restore elevation and rotation. Only the deltoid is required to be intact in the setting of a reverse total shoulder arthroplasty unlike an anatomic total shoulder that requires both the rotator cuff muscles and the deltoid. The design of the implant creates a fixed fulcrum that allows the shoulder to pivot using only the deltoid muscle. In a normal shoulder, the rotator cuff muscles will provide this fulcrum dynamically. After surgery, patients will have restoration of the ability to raise the arm overhead as well as use the arm in space in front of them. The only common limitation is internal rotation behind the back with average internal rotation restricted to the middle belt loop of a pair of pants.
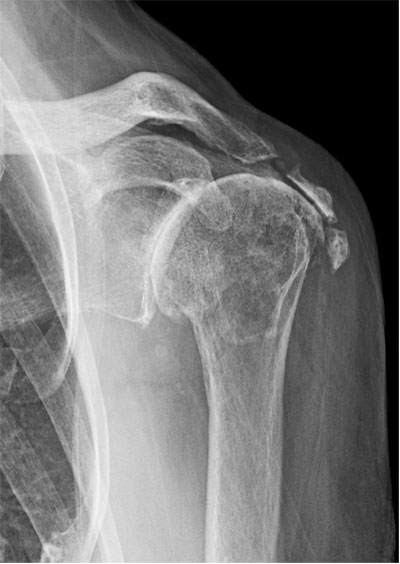
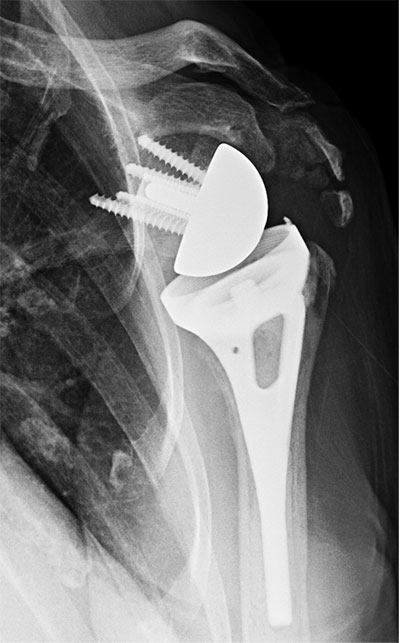
Rotator cuff arthropathy (shoulder arthritis with an irreparable rotator cuff tear) treated with a reverse total shoulder arthroplasty
Since its introduction in 2004 in the U.S., indications for reverse total shoulder arthroplasty have expanded to include the treatment of irreparable proximal humerus fractures, glenohumeral arthritis in the setting of severe glenoid bone loss or proximal humeral bone loss requiring bone grafting, failed treatment of proximal humerus fractures after nonoperative care or open reduction internal fixation and revision shoulder arthroplasty in the setting of failed hemiarthroplasties, anatomic total shoulder arthroplasties or reverse total shoulder arthroplasties. Bone grafting procedures on the glenoid or humerus are performed frequently using either autograft or allograft. Tendon transfers are often done at the same time as the reverse shoulder arthroplasty (latissimus or teres major transfer) in the setting of severe external rotation weakness to improve the ability to restore not only elevation but also rotation of the arm. Our team has evaluated outcomes of my patients after primary reverse total shoulder arthroplasty, RSA with bone grafting procedures on the humerus and glenoid and revision reverse total shoulder arthroplasty showing surgery can reliably restore pain relief and functional outcomes even in the setting of severe bone loss, failed fracture treatment or failed implants. (See images below of previously mentioned cases)
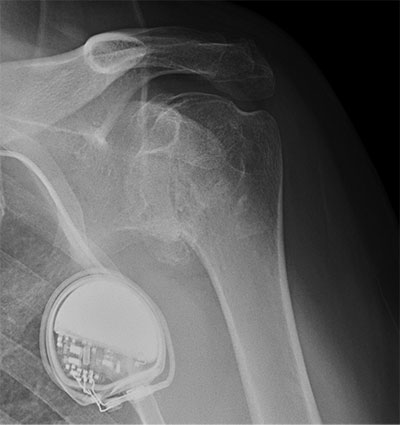
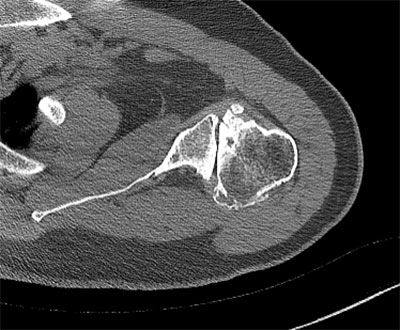
Primary glenohumeral osteoarthritis with severe erosion of the glenoid
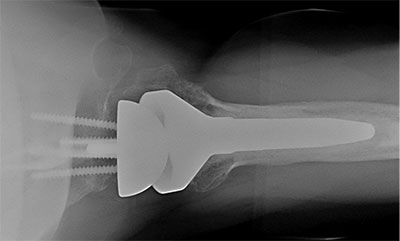
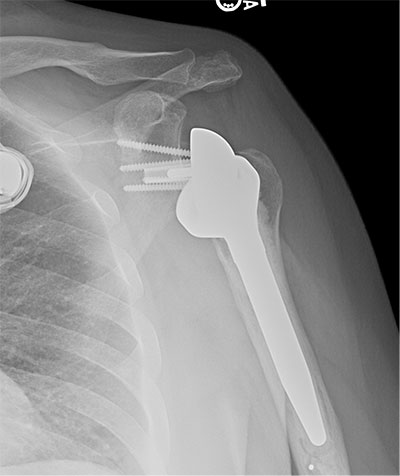
Reverse total shoulder arthroplasty of prior patient (axillary view and AP view) using humeral head autograft for severe glenoid erosion using a BIO-RSA technique

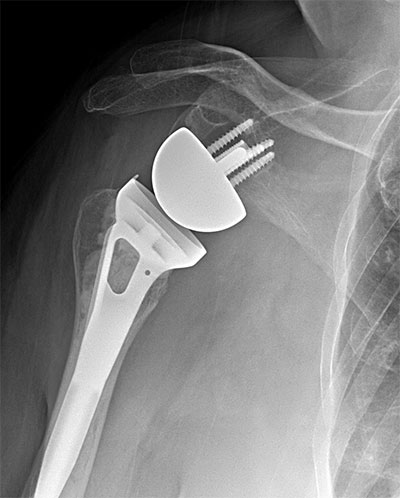
Avascular necrosis of the humeral head with severe proximal humeral deformity treated with reverse shoulder arthroplasty
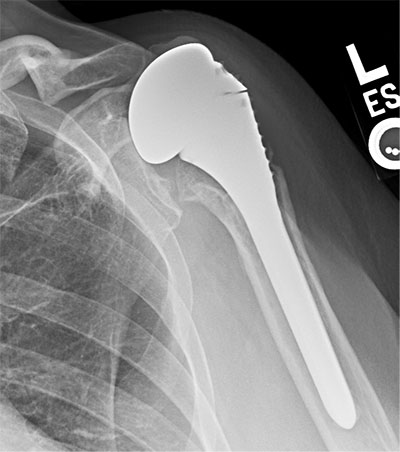
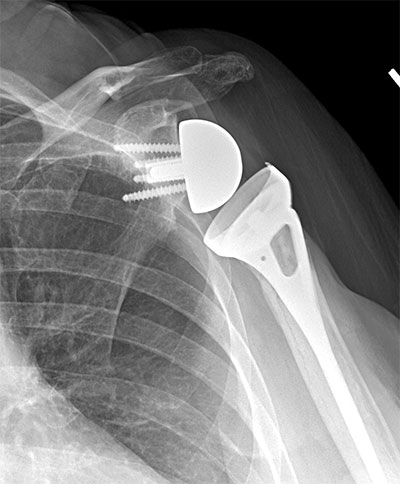
Failed hemiarthroplasty for fracture with rotator cuff insufficiency treated with removal of hemiarthroplasty and placement of a reverse total shoulder arthroplasty
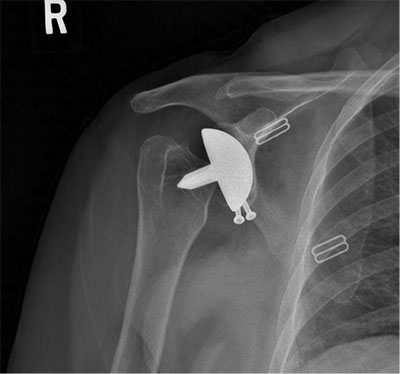
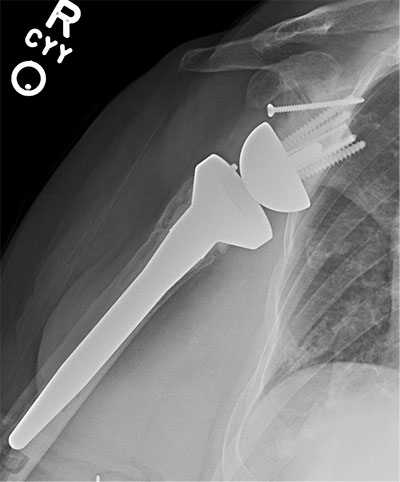
Failed loose humeral resurfacing with failed glenoid bone graft treated with revision removal of the resurfacing and placement of a reverse total shoulder arthroplasty with glenoid bone grafting using a femoral head allograft
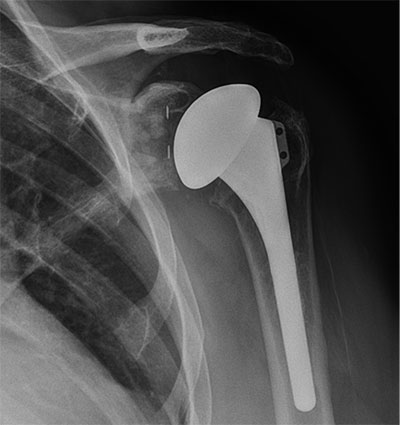
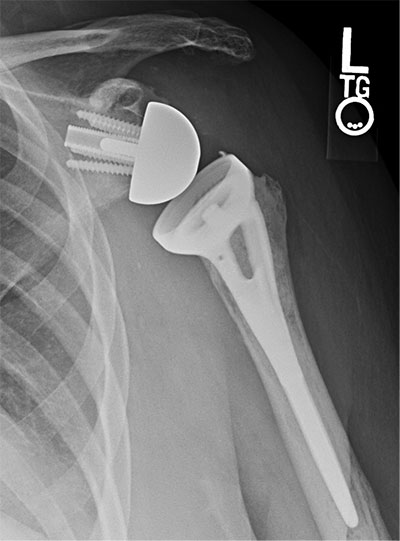
Failed anatomic total shoulder arthroplasty with a loose glenoid and cavitary glenoid bone defect converted to a reverse total shoulder arthroplasty with structural glenoid grafting using a femoral head allograft
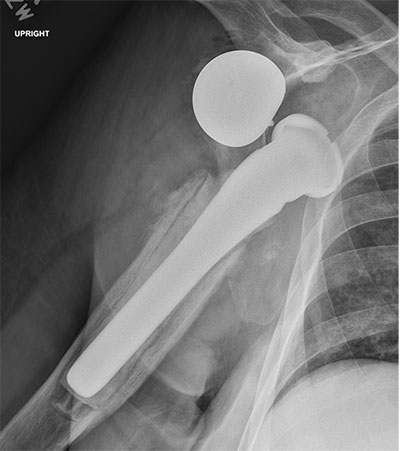
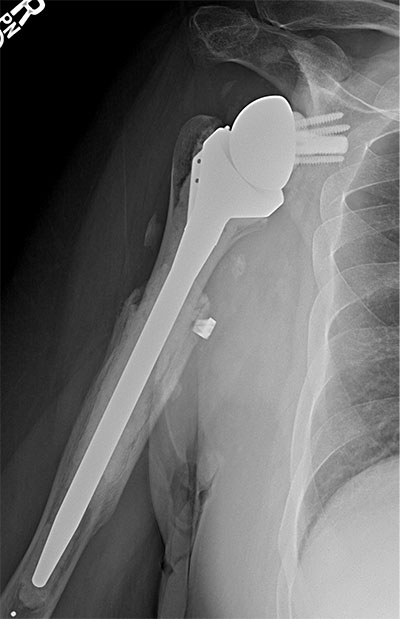
Chronically dislocated reverse total shoulder arthroplasty with severe proximal humeral bone loss treated with revision reverse total shoulder arthroplasty augmented with a proximal humeral allograft and metallic augmented baseplate

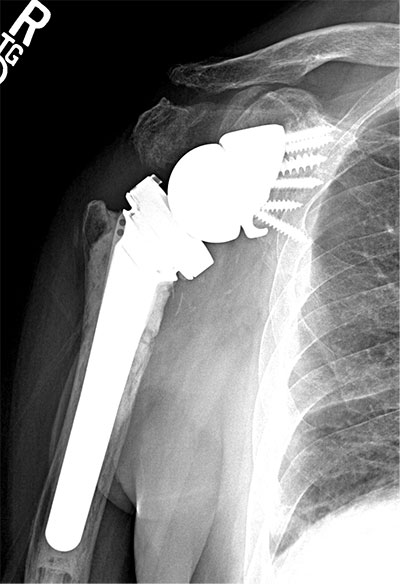
Failed Reverse Total Shoulder arthroplasty with humeral implant fracture and malpositioned baseplate and glenosphere treated with revision reverse total shoulder arthroplasty with humeral component revision and a custom metal augmented baseplate and glenosphere.
Indications for anatomic total shoulder arthroplasty or reverse total shoulder arthroplasty
- Endstage glenohumeral arthritis resistant to nonoperative treatments that cause significant shoulder pain, limit shoulder function or impair overall quality of life.
- Failed prior treatment of proximal humerus fractures either with nonoperative care, open reduction and internal fixation or arthroplasty
- Failed prior shoulder arthroplasty (hemiarthroplasty, anatomic total shoulder arthroplasty, reverse total shoulder arthroplasty) due to infection, fracture, dislocation, loosening of implants, instability, rotator cuff tearing, loss of range of motion
- Common symptoms include pain with activity and overhead use, pain at rest or sleep, weakness, loss of ability to raise the arm or place the hand in space
Evaluation for Shoulder Arthroplasty
The standard evaluation for a shoulder arthroplasty includes taking a full history and physical examination by the surgeon. Comorbidities will be discussed and optimized including prior cardiac events, blot clots, stroke, sleep apnea, sleeping, obesity, smoking, diabetes and any pulmonary issues. Preoperative evaluation will often include an evaluation by the patient’s primary care provider or cardiologist if there is a history of heart attack or abnormal heart rhythm. If the patient is on blood thinners, these will be stopped prior to surgery and typically restarted the night of the operation. Modifying agents for the treatment for inflammatory arthritis will be stopped prior to surgery based upon the specific medication.
Preoperative imaging will include a standard set of xrays of the shoulder as well as a CT scan of the shoulder for preoperative templating. An MRI may be obtained as well specifically in the setting of anatomic total shoulder arthroplasty to confirm the rotator cuff is intact. In the case of failed prior shoulder arthroplasty that needs revision, the patient will also have labwork (ESR, CRP) and a shoulder aspiration performed under fluoroscopy to rule out infection. If the labwork suggests a possible infection, the patient may require an arthroscopic or open biopsy prior to final revision shoulder arthroplasty. An EMG/NCV study may be required if there is any evidence of neurologic injury on physical examination. Finally, a standard set of lab work including a blood count, clotting factors and electrolytes will also be obtained. It is extremely rare to require a blood transfusion after shoulder arthroplasty so a type and screen will only be performed in select cases of patients at risk for bleeding or the need for transfusion.
Shoulder Arthroplasty Procedure
Whether the patient is to undergo a hemiarthroplasty, anatomic total shoulder arthroplasty or reverse total shoulder arthroplasty, the process is very similar. Patients are asked to wash their shoulder with hydrogen peroxide for several days prior to the surgery. We also utilize a preparation at the time of surgery for the skin including alcohol, hydrogen peroxide and Chloraprep or Duraprep which we have published showing that the combination reduces the incidence of bacterial contamination associated with the procedure. (Hydrogen peroxide skin preparation reduces Cutibacterium acnes in shoulder arthroplasty: a prospective, blinded controlled trial. J Shoulder Elbow Surg. 2019 Aug;28(8):1554-1561. doi: 10.1016/j.jse.2019.03.038. Epub 2019 Jun 20.)
The procedure is performed through an open incision approximately 8 cm long in the front of the shoulder. In an anatomic total shoulder arthroplasty, the front rotator cuff is taken down with a piece of bone for later repair. The humeral bone is then prepared using instruments and then glenoid socket is smooth, prepared and the plastic cup is placed and cemented. The humeral implant is then placed, and the front rotator cuff and the piece of bone attached to it are repaired back to the humerus using a combination of suture and small wires. In a reverse shoulder arthroplasty, the same incision is used. The front rotator cuff is taken down as a soft tissue sleeve. The humerus is prepared. The glenoid is then prepared and a small metal plate is screwed into placed on the face of the glenoid and a half of a sphere is then impacted on top of the plate and secured with a screw. The humeral component is then placed which includes a plastic cup and then the front rotator cuff is repaired with suture.
Postoperative Shoulder Arthroplasty Care
Surgery is inpatient and patients will stay overnight typically one night in the hospital. They may require further nights due to medical comorbidities or if they require discharge to a skilled nursing facility. All surgeries are performed under general anesthesia. Postoperatively, all patients are offered a nerve block by our anesthesia pain team. We will typically use either a peripheral nerve block (suprascapular nerve) or interscalene nerve block dependent on patient comorbidities. All patients will have a sling with a pillow that they will wear during the day and night and will only come out to perform exercises. Anatomic total shoulder arthroplasty patients will be instructed on shoulder, elbow, wrist and hand exercises while reverse total shoulder arthroplasty patients will only be instructed on elbow, wrist and hand exercises. The dressings may be removed at 5 days postoperative and the wound may get wet. Patients may let the arm down in the shower, let the water run over the shoulder, no soaping or scrubbing and then pat dry the wound. At that point, the patient does not need any dressings on the wound and will return to the clinic in 2 weeks from surgery for staple removal. Patients should contact our office (801-587-7158) for any signs of redness, swelling, drainage, increasing pain, fevers, numbness or tingling in the hand or fingers and be seen sooner than 2 weeks.





